The When of Eating: The Science behind Intermittent Fasting

The world is getting fatter. It’s a general trend, but one that’s especially well illustrated in the United States. As of 2018, 42 percent of US adults were obese — almost three times more than in 1980 and prior decades, according to government statistics. With that comes rising rates of serious health problems, including diabetes, atherosclerosis, heart attacks and strokes.
One reason for all this weight gain is that American adults are consuming more: National figures suggest an increase of around 200 daily calories between the early 1970s and 2010. Another is that many are snacking like never before. US adults ate about 20 percent more of their daily calories as snacks in 2010 compared with the early 1970s, and many no longer observe the traditional three daily meals. One 2015 study of 156 US adults found that most ate more than four times a day, and some up to 15 times, with an average of about six.
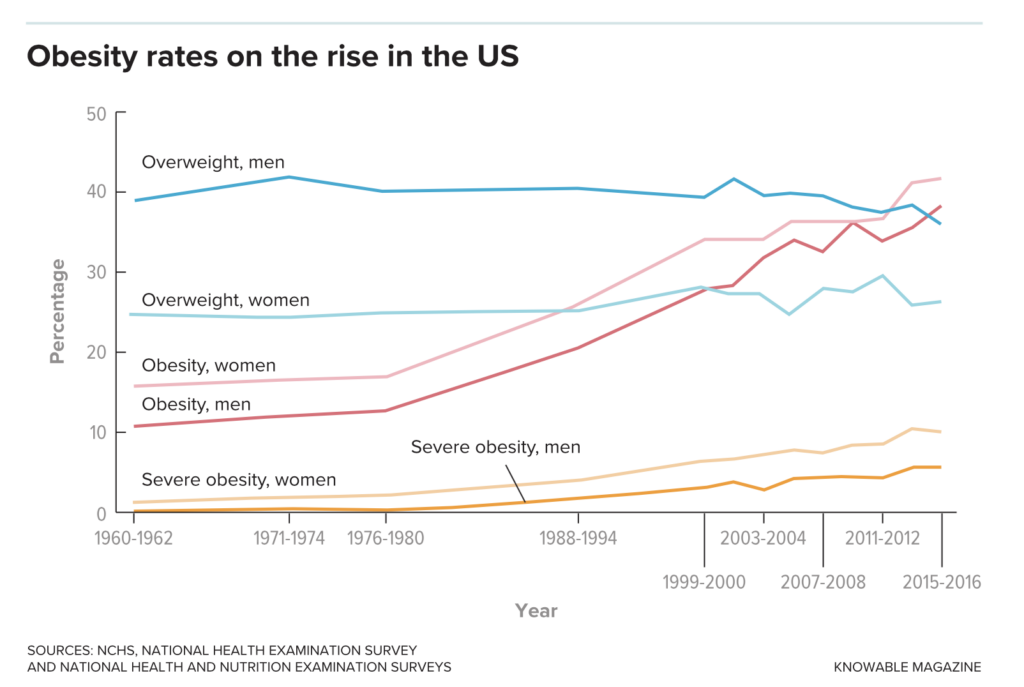
In the past 50 years, obesity has become much more common in the United States, with the latest estimates classifying 42 percent of adult Americans as obese.
(Obesity is defined as a body mass index of 30 or greater; severe obesity as 40 or more. Overweight is 25-29.9.)
But an increasing number of researchers think there is more to the rising rates of obesity than endless grazing. What also matters is timing: We eat when we shouldn’t, and don’t give our bodies a long enough break in between.
We didn’t evolve to eat many small meals day and night, says Dominic D’Agostino, a neuroscientist at the University of South Florida who studies the effects of nutrition on the brain. Instead, people evolved to deal with regular fasts: Until the dawn of agriculture around 12,000 years ago, we subsisted on hunting and gathering and often had to perform those activities with empty bellies. “We are hard-wired,” D’Agostino says, “to undergo periodic intermittent fasting.”
What’s more, these days people are eating at times of the day when historically they would have been asleep, says Satchin Panda, a circadian biologist at the Salk Institute in La Jolla, California, who wrote an overview on the timing of eating in the 2019 Annual Review of Nutrition. For thousands of years, he says, our nightly fast probably started much earlier than in these times of late-night TV and other electrified diversions (Zoom sessions, anyone?) that give us reason to stay up late and eat into the wee hours.
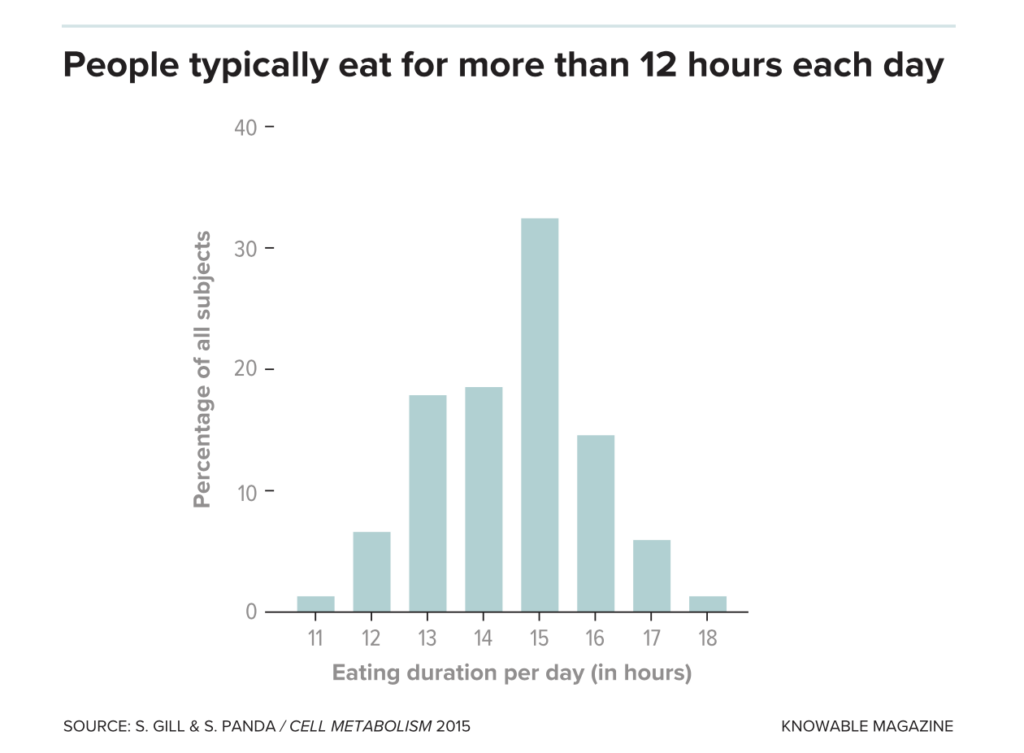
A 2015 report coauthored by Satchin Panda asked participants to digitally track everything they ate.
The timestamped data revealed eating often extends into the night, and that most people’s nightly fasts last less than 12 hours.
The timing of eating matters for body weight and health, studies are starting to suggest. Though the research is still mixed, heavily animal-dependent and often hard to parse, the literature shows significant potential benefits from fasting every other day or so — or, on a daily basis, eating only when we would normally be awake, within a window of 12 hours or fewer, a practice known as time-restricted eating.
Such practices — which have attracted thousands of followers and are often referred to under the umbrella term “intermittent fasting” — seem to help ward off obesity, proponents say, and may alter the body’s metabolism in healthful ways. More speculatively, there are signs in animal studies that the regimens might enhance athletic endurance and cognition, improve diabetes and perhaps even help to prevent or retard other medical conditions, such as cancer (see “Could fasting or ketone diets help quash cancer?”) and Alzheimer’s disease.

Feast or famine
How Americans became a nation of snackers is complicated, but part of the problem is rooted in studies, starting in the 1960s, that found links between metabolic benefits, weight loss and eating many small, nutritious meals throughout the day. Nibbling advice became a health mantra, partly based on the belief that frequent eating revs up the metabolism and makes the body burn more calories. This could be one of the reasons why “lots of people are now eating for 16 hours a day,” says biochemist Valter Longo, who studies genetics and nutrition at the University of Southern California.
Newer human research suggests that the mantra was ill-advised. It finds no support for the notion that endless nibbling increases metabolic rate, says Antonio Paoli, who studies the health effects of nutrition and exercise at the University of Padova in Italy. Quite the opposite: One 2017 study that followed more than 50,000 members of the Seventh-day Adventist Churches in the US and Canada found that people who ate three or more times per day gained more weight per year (as measured by the change in their body mass index over time) than those who confined their eating to one or two meals per day.
So could breaks between meals actually be good for one’s health? Studies as far back as the 1940s have reported that regimens akin to intermittent fasting improved health and prolonged lifespan in animals like rats. But it was unclear whether the animals were healthier because of the breaks themselves, or because the regimen caused them to consume fewer calories.
One of the first hints that pauses in eating are healthy in and of themselves came from a 2003 mouse study led by neuroscientist Mark Mattson, who at that time was working at the US National Institute on Aging. He and his colleagues fed one group of mice every other day and compared it with a group fed every day. (The two groups ended up eating essentially the same amount of food overall.) Researchers also followed another group, which ate 40 percent less.
After 20 weeks, the mice in the first two groups weighed about the same. But, strikingly, the alternate-day-fasting mice were healthier than the daily eaters, as was the fewer-calories group: They had lower blood sugar and insulin levels, signs that the pancreas is working more efficiently and suggesting that intermittent fasting might help to ward off diabetes.
The study also suggested brain benefits from intermittent fasting. When the scientists injected a nerve-damaging agent into the mouse brains, fewer nerve cells died in the alternate-day-fasting mouse group than the other two groups.
This added to earlier work by Mattson in which rats fasting every other day for three months had more nerve cells in the hippocampus, a brain region involved in learning and memory, than animals fed daily, as well as higher levels of a nerve-protecting chemical called BDNF. (That work stopped short of linking the benefits specifically to the pauses in eating, however — the design of the study didn’t permit that assessment.)
These findings were the first indication that intermittent fasting might improve brain function, which from an evolutionary perspective makes sense, says Mattson, now at Johns Hopkins University. After all, when an animal is in a state of hunger, it needs the brain to stay sharp so it can find food.
Mattson’s later work suggested a mechanism: The increased brain levels of BDNF he had seen in alternate-day-fasting rats can increase the number of mitochondria, the cell’s energy factories, in neurons. “Fasting is a mild energetic stress, and the neurons respond adaptively by increasing mitochondria,” he said in a 2014 TEDx talk at Johns Hopkins that has been viewed more than 4 million times. The mitochondria help the nerve cells produce more energy, boosting the maintenance and formation of synapses, the vital connections between nerve cells.
Is periodic fasting just like eating less?
If Mattson’s findings in animals could be replicated in people, they would suggest that fasting every other day or so holds benefits beyond cutting calories. Such studies are difficult, however. Trials in which people eat less or nothing every other day, or every few days, consistently show weight loss and improved cardiovascular health. But you can get similar results simply by cutting calories. It’s been hard to prove that the timing of eating is what matters.
In the longest human trial reported so far, nutrition researcher Krista Varady of the University of Illinois at Chicago and her team randomly assigned 100 otherwise healthy obese people to do one of three things for six months (followed by a six-month maintenance phase): eat just 25 percent of normal every other day (on non-fast days, they got to eat 25 percent more than their needs); eat 75 percent of their calorie needs each and every day; or eat normally, as a control group. Since overall calorie reduction was equal in groups one and two, any edge that the first group had could be put down specifically to intermittent fasting.
But the study, published in 2017, found no difference between groups one and two: They lost the same amount of body weight on average (about 7 percent after the six-month dieting phase), and displayed similar measures for risk factors for heart disease and diabetes such as blood levels of cholesterol, sugar or insulin; or the body’s responses to insulin. That the intermittent fasting offered no additional benefits beyond traditional calorie restriction was “pretty disappointing,” says nutrition scientist Courtney Peterson from the University of Alabama at Birmingham.
Varady’s study also suggested that fasting every other day is harder for people to stick with than cutting calories across the board. The intermittent group had slightly more dropouts than the calorie-cutting group (about one-third versus one-quarter, respectively) and would stray from the regimen, overeating on fast days and undereating on feast days. “On the fast days, some people felt pretty hungry,” Varady says.
Eating in sync
Another strand of research suggests that restricting when we eat to only certain times of the day — ones when our species would normally have been awake — might be easier to stick with than periodically fasting for an entire day, and offer some of the same health benefits.
The first indication that timing of eating matters for health came from two studies, one in rodents and one in people. The rodent one, published in 2009 and led by sleep researcher Fred Turek at Northwestern University, showed that mice fed a high-calorie diet during the day (when the nocturnal animals would normally be asleep) gained a lot more weight than mice fed the same diet during the night (the creatures’ active hours). This happened even though the animals consumed the same number of calories overall.
The same year, neuroscientist Frank Scheer of Brigham and Women’s Hospital in Boston reported that putting people on an artificial, 28-hour “day” in a lab for 10 days (so that they often ate at times when they would normally be sleeping) led to increased blood pressure and levels of blood sugar and insulin. “That study,” Peterson says, “was a huge watershed study because it showed, literally, that the time when you eat affects your health.”
If eating when the body should be sleeping is unhealthy, then it follows that restricting eating to waking hours might be healthy. That’s what Panda’s team showed next. In studies published in 2012 and 2014, they reported that mice fed a calorie-dense diet during windows of eight to 12 hours at night (the animals’ active time) were protected from becoming obese and gained less weight than mice able to eat at any time — even though, again, both groups ate the same number of calories overall.
Restricting eating to just nine hours at night even caused obese mice to lose weight. It also lowered their blood sugar and improved glucose tolerance (the insulin-driven movement of sugar from blood into cells), suggesting that time-restricted eating might help to alleviate or prevent diabetes.
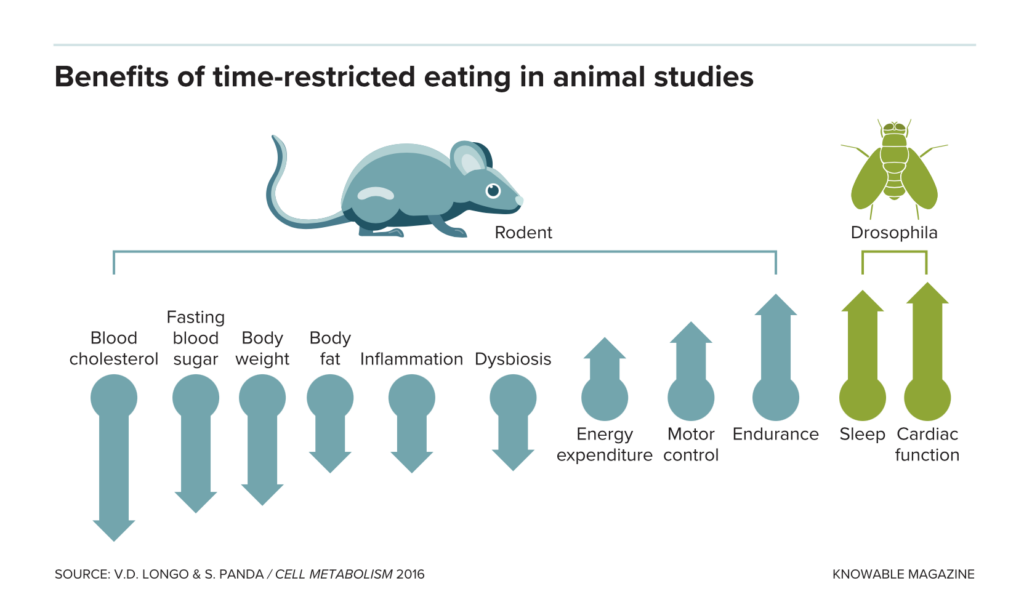
In rodents, limiting eating to an eight-to-12-hour window at night, when they are naturally active, leads to benefits in many different body systems, from reduced cholesterol, inflammation and microbial imbalance in the gut (dysbiosis) to increased endurance compared with others allowed to eat the same chow at any time. Drosophila fruit flies improve in sleep and heart health when fed only for 12-hour spans during the day.
The findings suggested that time-restricted eaters must somehow metabolize incoming calories in a way that’s better for the body, Panda reasoned. And indeed, he and colleagues found — also in mice — that time-restricted eaters excrete more sugar and cholesterol breakdown-products in their feces (a sign of a more healthful metabolism) than the mice fed at the “wrong” times of the day.
But just as with alternate-day fasting, it’s been difficult to show in people that the effects of time-restricted eating are due to anything more than old-fashioned calorie restriction.
For example, in a trial published in 2018, Varady asked 23 healthy, obese people to eat only during an eight-hour window between 10 a.m. and 6 p.m. for 12 weeks. Participants lost about 3 percent more of their body weight, on average, than controls who ate as usual, and also ended up with lower blood pressure.
But the eight-hour eaters also ate 300 calories less per day, making it impossible to tell whether the health benefits came from reduced calories, time-restricted eating or both.
So for now, it’s unclear whether Panda’s mouse findings fully apply to people. “It sounds too good to be true,” says research dietitian Michelle Harvie of Manchester University NHS Foundation Trust in the UK. One human study published in 2007, she says, even suggested that restricting eating times too much can be bad: In it, people ate all their calories in a single meal between 4 p.m. and 8 p.m. Blood sugar levels rose, and glucose tolerance worsened, both signs of ill health.
A recent, randomized, controlled study in overweight and obese people also showed no improvement from restricting eating times to the eight hours between noon and 8 p.m. Over 12 weeks, the 59 time-restricted people lost about two pounds on average, not significantly more than the average 1.5-pound loss in 57 controls. And when the researchers looked at 46 of the 116 total participants in more detail, the restricted group showed no improvement in blood sugar or insulin levels and lost more of their weight from lean mass (sources other than fat that may include water and muscle) than controls did.
For Ethan Weiss, a cardiologist at the University of California, San Francisco, who led the study, the findings were disappointing enough to stop the time-restricted-eating regimen he had been following for seven years, he wrote on Twitter.
Still, some researchers think the problem with such disappointments might lie in timing. More specifically, Peterson suspects that in both these studies, the last daily meal might have been consumed too late, when blood insulin levels (which rise and fall in cycles) had dropped too low to process food properly. (For the same reason, Paoli says, rich people in the 19th century were in bad shape: They got up at noon and had their last big meal at midnight or 2 a.m.)
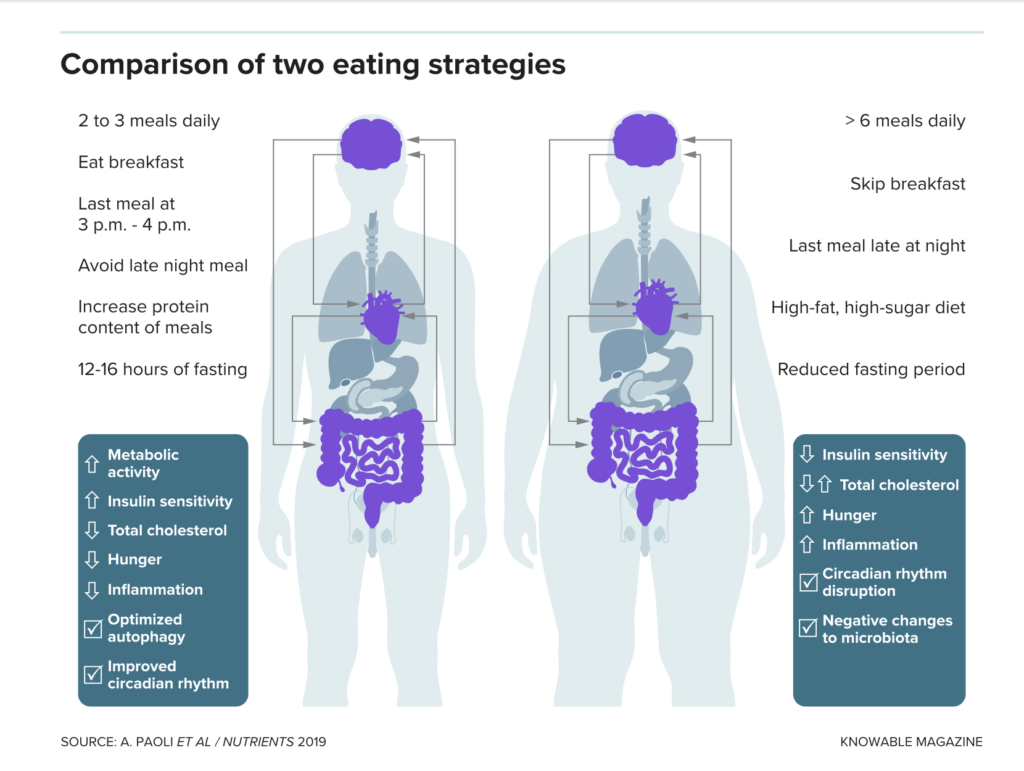
Studies in people have shown that many markers of health improve by eating fewer, protein-rich meals within a shorter window of time, compared with consuming six or more meals of a high-fat, high-sugar diet with a short nightly fast. (Autophagy is a cellular process that plays an important role in normal cardiovascular function. Interactions among brain, heart and gut are important in these responses.)
In 2018, Peterson and her colleagues reported results from a study of eight overweight prediabetic men asked to eat all their food within a six-hour window — but on an earlier schedule, with dinner before 3 p.m. After five weeks, neither these men nor those in a control group with a 12-hour eating window lost weight — in fact, the study was deliberately set up to avoid weight loss, in order to test for independent benefits. But otherwise, the six-hour group was healthier: Blood pressure was lower and blood sugar levels were better controlled.
And this time, the calories both groups consumed lined up. This makes the study, while small — Peterson plans to repeat it with more people — the first controlled human trial that seems to jive with Panda’s mouse findings. If confirmed, it suggests that restricting eating to a window of less than 12 hours while we are awake does have health benefits independent of calorie reduction or weight loss.
Timing, timing, timing
But what time window is best for eating? For many of us, breakfast is the easiest meal to skip. Indeed, an increasing number of people do just that to lengthen their nightly fast and (they hope) reap health benefits. For that reason, Peterson next wants to compare the effects of two seven-hour eating windows — one early in the day and the other in the middle of the day— in the hopes that skipping breakfast is a win.
And what’s going on in the body to make it healthier to eat at one time than another? Daily biological rhythms may be central here, says Dorothy Sears, an obesity researcher at Arizona State University who wrote about the metabolic effects of intermittent fasting in the 2017 Annual Review of Nutrition. It’s during the day that your body is best able to process food, she says.
Food-processing organs such as the liver or pancreas follow 24-hour rhythms, notes Panda. During the day, the pancreas is best at secreting insulin to tell the liver to take sugar from the blood and store it as glycogen and fat. Before bedtime and at night, it’s programmed to slow down insulin secretion. Even the bacteria that live in our guts follow a daily rhythm, with likely effects on health and digestion.
And just as the brain needs rest at night to do much-needed repair and cleanup work, Panda says, so does the body — to break down cholesterol, damaged mitochondria or misfolded proteins, for example. But should you sneak to the refrigerator at a time when you normally sleep (for most people, that would be at night), cells and organs must abandon their planned cleanup to process food and store up fat. If this happens too often, Panda says, such “metabolic jet lag” can lead to weight gain and other health problems, even if calorie counts remain constant.
With circadian rhythms in mind, Panda recommends that people avoid eating for an hour or two after they habitually wake (because high morning levels of cortisol and melatonin reduce insulin action), and for three hours before they habitually go to bed (after that, the hormone melatonin inhibits insulin production and the gut moves more slowly). Panda stresses the word “habitually,” because natural wake times differ depending on whether people are morning larks or night owls.
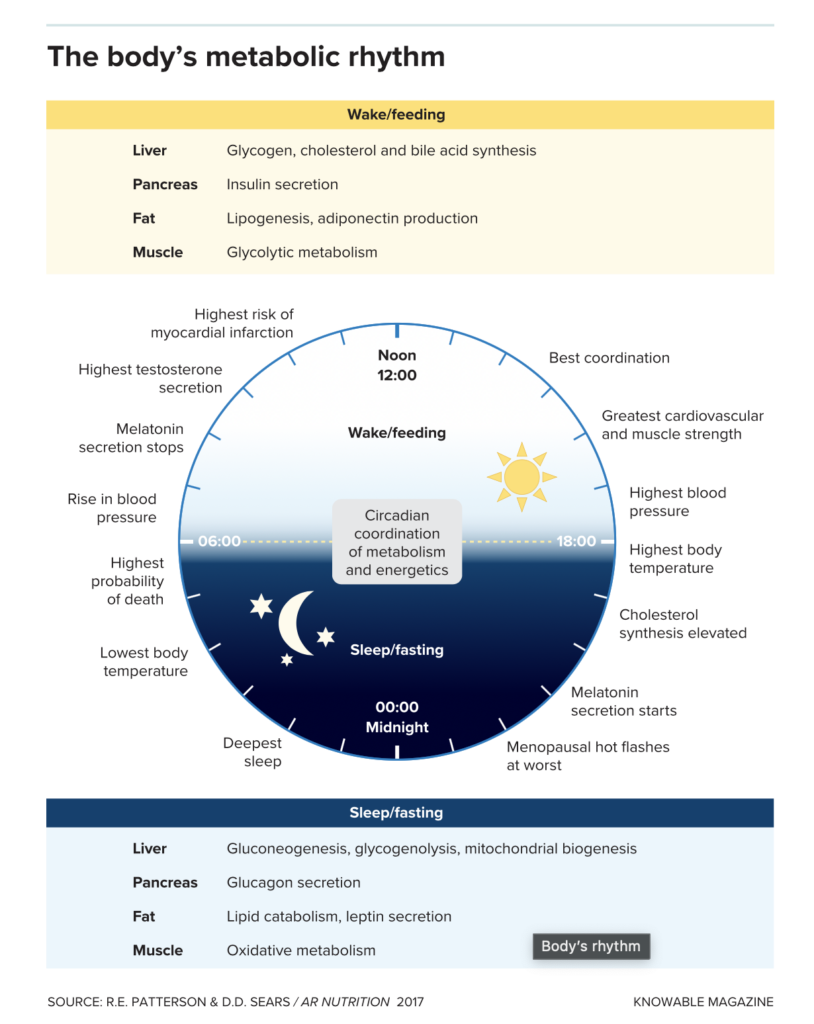

The body’s internal rhythms follow a roughly 24-hour cycle, which influences hormones, metabolism, physical activity, sleep and more. The planet’s light-dark cycle helps keep the body clock in step with day and night. Eating can also affect the rhythm. Time-restricted feeding seeks to align meal times with the wakeful phase of the cycle.
Panda also hopes that such time-restricted eating may be feasible for people to stick with. He and his colleagues recently had 11 healthy overweight or obese people who normally spread their meals over 15 hours try to restrict daily eating to an eight-hour window. Using a food and activity tracking app Panda’s team developed, the participants lost 3.7 percent of their body weight on average over 12 weeks, while nine controls lost only 1.5 percent on average, though this was not a statistically significant difference.
In an earlier study, Panda found that overweight people were willing to restrict their daily eating times to 10 or 11 hours for a year. Perhaps that’s because they also reported better sleep and feeling more energetic, Panda says. He says that more recent (as-yet-unpublished) data from thousands of additional people using his app confirm that study’s conclusions.
Is fasting longer always better?
When we fast, our bodies run on stored energy. Initially, that energy comes from glycogen, the stored form of glucose found in the liver and the muscles. But once we’ve fasted for some time, the liver runs out of glycogen and switches to producing chemicals called ketone bodies from metabolizing fat. The mitochondria then use these ketone bodies instead of glucose to get their energy.
This means that if we extend our nightly fast beyond about 12 hours, say Panda and Mattson, our bodies lose weight by burning fat, something that most of us would probably consider a good thing. It is this “metabolic switch” from burning glucose to burning fat and the resulting elevated levels of ketone bodies in the blood that accounts for some of the health benefits of intermittent fasting, Mattson says.
So should we try to fast for as long as we can each night? Longo notes that we don’t yet know whether regular fasting for more than 12 hours every day is good for people over the long haul. There are no long-term human studies, but one small study in rats found that glucose tolerance initially improved but then worsened as the months wore on.
Longo also thinks that periodically fasting for too many hours might ultimately lead to problems such as gallstones. That’s because fats and cholesterol can accumulate, generating stones in the gallbladder. One study of 4,730 women published in 1991 found that overnight fasts of more than 14 hours roughly doubled the risk of hospitalization for gallstones compared with seven-hour nightly fasts.
What’s more, physicians have long viewed the state of ketosis as potentially dangerous, because high ketone concentrations make the blood acidic. If left untreated, this “ketoacidosis” can damage the liver, kidneys and brain, and even kill. The condition mostly occurs when people with type 1 diabetes don’t get their insulin medication in time. Since they can’t make their own insulin, the liver starts burning fat and generates ketones.
But the picture is different for healthy people who can still make insulin. A ketogenic diet — high in fat, low in carbs — has long been used to reduce seizures in children with epilepsy. And though medical experts still flag the potential risks (such as stressing the kidneys or perturbing our gut flora) and urge caution, their acceptance of low-carb diets — and the elevated ketones that come with them — has grown over time. In healthy, non-diabetic people, D’Agostino says, elevated ketone levels are natural, an evolutionary adaptation that enabled us to keep the brain running when food was scarce, because the brain’s mitochondria can use ketone bodies as an energy source instead.
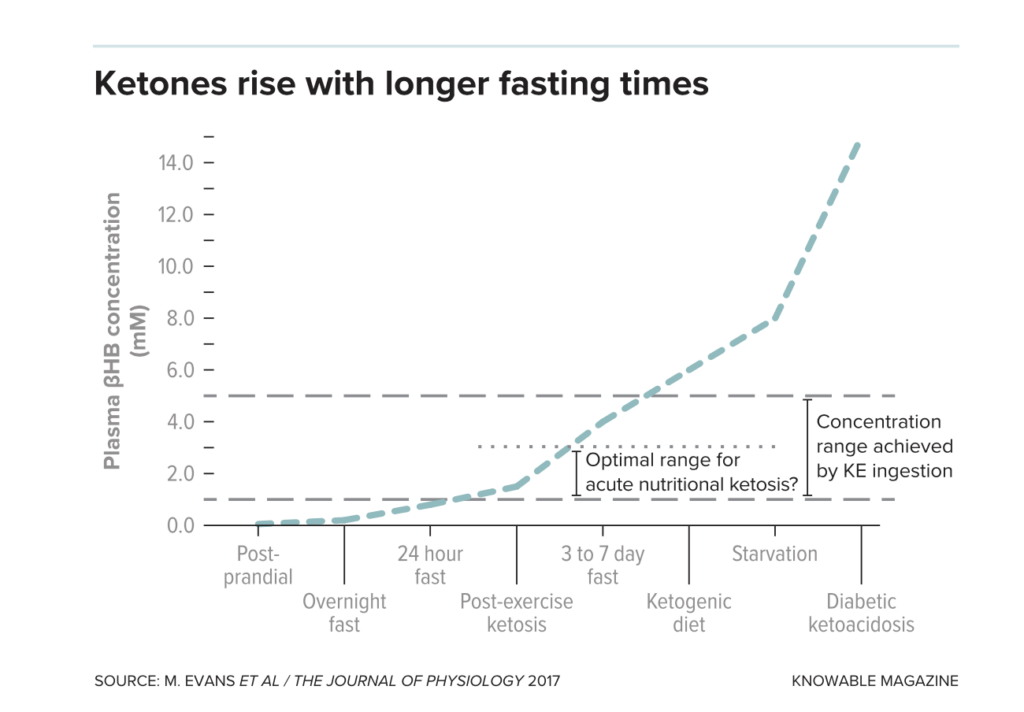 After a meal (post-prandial), ketone body levels in the blood are at their lowest. But they rise during fasts or after exercise. Ketone ester (KE) drinks or following a ketogenic diet also boosts levels. At the high levels seen in starvation and ketoacidosis, ketones can become a danger. Researchers speculate that an optimal range to improve athletic performance can be reached with a KE drink.
After a meal (post-prandial), ketone body levels in the blood are at their lowest. But they rise during fasts or after exercise. Ketone ester (KE) drinks or following a ketogenic diet also boosts levels. At the high levels seen in starvation and ketoacidosis, ketones can become a danger. Researchers speculate that an optimal range to improve athletic performance can be reached with a KE drink.
A gain for the brain?
Indeed, D’Agostino and Mattson would go so far as to suggest that elevated ketone levels help to boost brain function. D’Agostino has reported that a ketone ester drink helps to stabilize brain chemistry in mice with a genetic condition that causes seizures as one of its symptoms, such that levels of one brain chemical called GABA (which has a calming effect on brain activity) increased, while levels of another called glutamate (which excites brain cells) went down. “Ketones,” D’Agostino declares, “bring the brain to a normal state.”
And in 2016, Mattson reported evidence suggesting that ketones might explain the enhanced numbers of brain mitochondria he had found in alternate-day-fasting rats. He suspects that ketones might also benefit people with Alzheimer’s disease, whose brain mitochondria can’t use glucose as efficiently to produce energy and who can experience seizures in the disease’s late stages. In late 2019, he reported ketone benefits in a mouse model for the neurodegenerative disease.
Mattson has also been testing the effects of intermittent fasting on brain health in people: One small trial he launched in 2015 had 20 overweight-to-obese people with insulin resistance consume just 500 calories for two days a week (eating normally other days) for two months; it aims to look for improved brain function and metabolism compared with 20 similar people who eat normally. (Results are expected later this year.)
Some proponents speculate that ketone-induced changes in the brain might be behind the improved focus people report when fasting: D’Agostino says the one time he fasted for seven days he wrote two grant proposals (both successful) and a key publication.
“Anecdotally,” says Mattson, “I get a lot of feedback from people who switched to intermittent fasting and claim that they are more productive and focused.” He says that the US Air Force and NASA have approached him to discuss how fasting might enable pilots or astronauts to focus for extended periods of time.
Better focus is why Geoffrey Woo, whose company HVNM has sold a ketone ester drink, got interested in fasting: In 2016, he started the group WeFast that holds regular fasting events in Silicon Valley to help people up their productivity — the group now has more than 20,000 members.
And the small but provocative studies keep coming. In 2016, biochemist Kieran Clarke at the University of Oxford reported that a ketone-rich diet improves spatial learning and memory in rats. Two years later, Brendan Egan and Mark Evans of Dublin City University reported that ingesting a ketone ester drink prevented the increase in decision-making mistakes often seen after exercise in field-sports players. Still, Egan cautions that in his more recent studies, a ketone drink did not improve cognitive performance in runners.
What about physical performance?
If the brain is enhanced by ketones or by fasting, so might physical performance. Panda’s mice ran nearly twice as long on treadmills with a 15-hour fast compared with a 12-hour one, for example; when Clarke fed rats a ketone-enriched diet for 5 days, the animals ran 32 percent further on a treadmill.
In people, the results are mixed. Egan found that eight weeks of a 16-hour nightly fast or ingesting a ketone drink did not improve measures of endurance, whereas Paoli says he has unpublished evidence of improved muscle efficiency in long-term intermittent fasters. And when Clarke gave a ketone drink along with sugar to eight cyclists to achieve ketone levels akin to one week of fasting, performance in a 30-minute time trial improved by 2 percent or the equivalent of about 400 meters, a significant difference for elite sports.
Quaffing a beverage may be easier than an intermittent fasting regimen, but it will cost you: HVNM’s now out-of-stock drink cost a robust $33 for a 65 milliliter-serving with 25 grams of ketones, equivalent to three to seven days of fasting, Woo says. Because ketones are made by the body, the ketone ester drink isn’t illegal in elite sports. (“There have been races won,” Clarke says. “I can’t say who.”) Woo says that most of the competitive cycling teams on the European Grand tours like the Tour de France and the Giro d’Italia have used the HVNM ketone ester drink before races.
Still, the drink is too expensive for many for daily use. (And, as an aside, there is the taste: When my wife tried it while training for the New York City Marathon a few years ago, she called it “disgusting, like acid reflux mixed with gummy bears.”)
Keeping at it is key
At this point, you might be wondering: What kind of fasting is best, be it to lose weight, enhance health or improve one’s mental or physical edge? Does this mishmash of experiments — in rodents, in athletes, in overweight people — suggest that long, nightly fasts are best, or fasting every other day? Or what?
One guide is to simply choose what’s easiest to stick with. Anecdotal evidence, along with some data on hunger and mood, suggests lower dropout rates for daily, time-restricted eating than for fasting every other day or a couple of days a week. “Time-restricted regimens are more sustainable,” says Mary-Catherine Stockman, a dietitian in Clarksville, Tennessee, who cowrote a 2018 review on the evidence about alternate-day-fasting regimens. “People tend to be more satisfied. That’s what I’ve seen with patients.”
And indeed, many of the experts interviewed for this story — who don’t themselves agree on every point and continue to debate the details and interpretations — restrict their daily eating times.
 Studies in flies, mice and rats have demonstrated metabolic benefits of restricting eating to a window of time in sync with the body’s natural activity and resting cycles. Emerging evidence from research in people also shows benefits of time-restricted feeding in curbing metabolic problems. Some think it may also boost brain health. (ETC stands for electron-transport chain; UCP is uncoupling protein.)
Studies in flies, mice and rats have demonstrated metabolic benefits of restricting eating to a window of time in sync with the body’s natural activity and resting cycles. Emerging evidence from research in people also shows benefits of time-restricted feeding in curbing metabolic problems. Some think it may also boost brain health. (ETC stands for electron-transport chain; UCP is uncoupling protein.)
Panda, who has published a book about his findings, fasts for 14 hours every night and eats only twice a day: breakfast, and then dinner before 6 p.m.
D’Agostino follows a ketogenic diet and doesn’t eat until noon or mid-afternoon — except for a glass of water with lemon and black coffee — on days with important work, in order to enhance his focus. “I feel sharper, more creative in that state,” he says.
Mattson fasts for about 18 hours every night: He eats only after a late-morning exercise session, to further boost his ketone levels. He says it takes about a month to adjust to such a regimen without getting hungry.
And Longo has developed (and occasionally follows) a “fasting-mimicking diet” that puts the body into ketosis while providing essential nutrients. The foods, whose ingredients are proprietary, are intended to be eaten for five consecutive days. In a three-month randomized trial of the Longo regimen reported in 2017, participants lost 2.6 kilograms (5.7 pounds) of weight on average and had lower blood pressure.
Other than that, Longo says it’s probably best to stick with the habits of certain centenarians who follow low-meat diets and regularly avoid eating for 12-hour stretches. “You really don’t see centenarians fasting for 16 hours a day,” he says.
All the unsettled points and lack of clear-cut evidence from human trials hasn’t stopped thousands of enthusiasts from experimenting with their own personal intermittent-fasting regimens, in large part because many find it easier to count hours than calories. And there’s hope it might become easier still, if what goes for mice goes for people: Panda’s rodent studies suggest that skipping weekends doesn’t ruin the time-restricted health effect.
“You think, ‘What about Saturday night, when I go out for a late dinner?’ In the mice, that is OK,” Sears says. “It’s very encouraging, because it seems that you don’t have to ask people to be perfect every day of the week…. And you don’t ever have to read a label.”
Sources:
Author:

Andreas von Bubnoff
Andreas von Bubnoff is a freelance science writer and professor of science communication based in Germany. He drinks his morning latte in a beer mug and likes to have breakfast at noon.





