Top 10 Secrets About Stress And Health

It’s no secret that stress is bad for your health.
Everybody knows that “life stress events” — things like loss of a job, death of a loved one and getting divorced (or married) raise the risk of getting sick.
All sorts of other life events also generate stress, with possible negative health effects ranging from catching a cold to major depression to a fatal heart attack.
Of course, knowing about the link between stress and sickness just gives you something else to worry about, adding even more stress. If you value your health, perhaps you should stop reading now.
On second thought, don’t. Much of the lore about stressful events impairing health is certainly true, but some research is reassuring. There are some secrets about the stress-disease connection that aren’t all bad.
If you’ve read the psychological, psychiatric and medical scientific literature over the last several decades, you might already be aware of these “secrets.” If not, they’ve been nicely summarized in a paper to appear in the next issue of Annual Review of Psychology, in which Sheldon Cohen, Michael L.M. Murphy and Aric A. Prather analyze (in no particular order) what they call the
“Ten surprising facts about stressful life events and disease risk.”
10. Experts disagree about what counts as stressful.
Nobody disputes that certain events inflict severe psychological (and physiological) stress. Death of a spouse, getting diagnosed with a terminal illness and (ahem) separation of children from parents are indisputably “major stressful life events.” But no clear rules have been established to define what features place an event in that category (which makes stress research complicated, with often ambiguous results).
Some researchers hold that stress magnitude hinges on how much “adaptation” is required to cope with it (which is why marriage can be considered especially stressful). A second theory gauges stressfulness as the amount of threat or harm an event poses. Some experts view stress as a mismatch between demands and resources. (If you have the resources — say, money — to address and control a demanding situation, it’s less stressful; if your boss expects you to complete a three-person project all by yourself under an impossible deadline, you’re stressed.) A fourth view regards “interruption of goals” as the prime feature of a life stress event; diabolically, one of the goals most commonly interrupted is the goal to be psychologically well.
These theories about stress-event criteria aren’t mutually exclusive, of course. “There is obvious overlap among these approaches,” Cohen and colleagues write. On the whole, though, they suggest the “threat or harm” perspective is the most commonly accepted.

Life events commonly included on stress questionnaires may be objectively bad or good, major or minor. They include the death of a spouse, divorce, the loss of a job — or even a big achievement. Some stress checklists focus more on traumatic events, such as assaults; others ask about events that in the last year have brought major or minor changes to everyday life, requiring adaptation or readjustments, even if they are seemingly beneficial (getting a promotion). Some important events related to illness are those that affect social status, self-esteem, identity and physical well-being. Not all are equal in effect, and there’s much variation in how people respond.
9. Stress can affect a long list of diseases.
Depression and heart disease are commonly associated with stressful events, but stress’s influence extends to other health problems as well. Many, perhaps even most, diseases can be linked to life stress in some way. Stress can boost anxiety, mess with your hormones and discourage healthy practices such as exercising and eating well. At the same time stress can instigate bad behaviors such as smoking and drinking. All these responses can have negative impacts on important organs (brain, heart, liver), possibly resulting in multiple health problems either by triggering the onset or accelerating the progression of a disease. Stress events can reduce resistance to infections, and even cancer may be linked to stress. But the evidence on cancer is less clear. Stress might influence the development of cancer, but the strongest research shows that a more likely effect of stress is reducing cancer survival rates rather than initiating cancer onset.
8. Just being stressed doesn’t mean you’ll get sick.
There’s no doubt that trauma and stressful events can harm your health. But not always. “On the whole,” Cohen and colleagues write, “most people who experience stressful events do not get sick.” Experiments exposing stressed and nonstressed people to a common cold virus found that more of the stressed people caught the cold than those in the nonstressed group, but nevertheless half the members of the stressed group remained healthy. Even depression is not an inevitable effect of major life stress; some people are more resilient than others. Positive self-image and sense of control are signs of resilience; negative attitude and excessive rumination tip the scales toward depression.
7. Stressful events do not strike at random.
Apart from the relatively rare natural disasters, fatal accidents and a few other nasty exceptions, stressful events are not equal-opportunity assailants. Your personal traits and situation and the circumstances in which you live make you more or less at risk for life stress. Neighborhoods with low socioeconomic status are sites of higher-than-average levels of stressful events, and people with low personal socioeconomic status have more risk of encountering violence, death of a child and divorce. Even personality can boost your stress risk (neurotic, unconscientious and disagreeable people are more likely to get divorced, for some reason). One study found that “individuals characterized by negative attributional style” (i.e., jerks) encounter more “interpersonal conflicts,” raising the risk of stressful events. Furthermore, one stressful event — such as loss of a job — can lead to others (such as loss of income, moving or divorce).
Evidence is strong that stressful events make a disease you already have worse.
6. Disease might come before the stress.
While some evidence supports the notion that stress can initiate various diseases, this may not be the case in truly healthy people. “Rather, events may influence risk for disease by either suppressing the body’s ability to fight invading pathogens or exacerbating the progression of ongoing premorbid processes,” Cohen and colleagues write. What looks like a disease triggered by stress “may actually be stressor-triggered progression of previously unidentified disease.” So in some cases stress might not be responsible for the disease itself, just for making a previously unnoticed disease worse.
5. Some stressful events are more powerful than others.
The magnitude of a stressful event’s impact depends a lot on the nature of the stress. Most damaging, research indicates, are “experiences that threaten an individual’s sense of competence or status,” striking at a person’s “core identity.” Loss of status, losing a job and interpersonal conflict with spouses or close friends can all exacerbate health problems, from raising the risk of depression to worsening high blood pressure and reducing resistance to respiratory infection.
4. Chronic stress is worse than acute stress, usually.
It’s not necessarily obvious that chronic, long-lasting or recurrent stress is worse than one-shot stress events. It may be possible to adapt to ongoing stress — once you’re used to it, maybe it won’t bother you so much (or harm your health). On the other hand, ongoing stress may be worse for health because it’s always there, ready to attack whenever your body is vulnerable for some other reason. Overall, chronic stress is probably worse, as it may have a persistent detrimental effect on the body’s disease-fighting immune system. Acute stress, like single traumatic events, may trigger a dramatic worsening of an existing condition, such as heart disease. In that case, a sufficiently powerful stress event can induce a fatal heart attack.
3. Many stress events are worse than fewer, maybe.
Effects from stressful events may add up over time; simple checklists of how many stressful events a person has experienced over the past year show that experiencing more events predicts worse health. But it’s too complicated to say exactly why that is, or even if it is really generally true. (The checklist method of gathering data might be faulty.) In fact, if a single event is strong enough to increase health risk substantially, additional events don’t necessarily increase that risk further. For that matter, it isn’t clear how events should be counted; a divorce followed by changing residences and reduced income might count as one event or three, Cohen and colleagues point out. And it may not be the number of events but rather the number of “life domains” in which you’re experiencing stress that’s more important. (Job, home life, medical issues and financial issues all represent different domains in which stress may occur.)
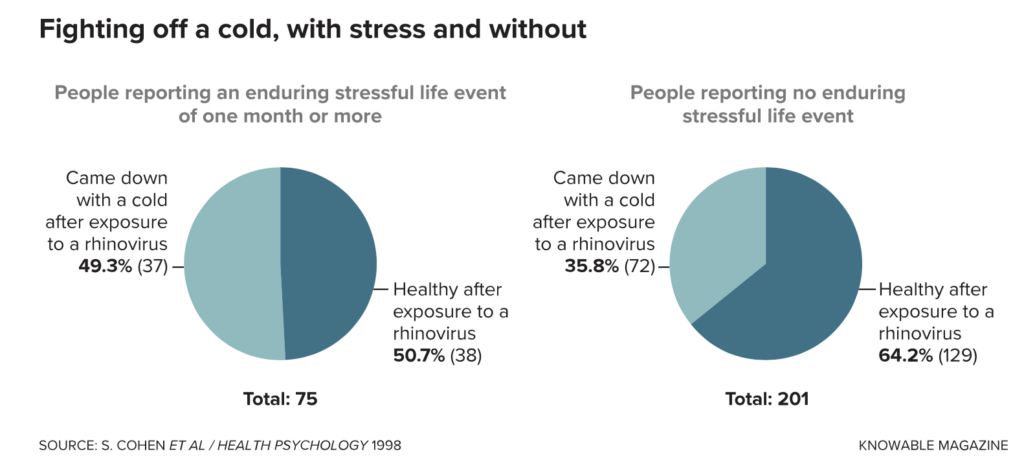
One study looked at how people’s self-reported experiences of stress influenced their ability to fend off exposure to a common cold virus called rhinovirus. Those reporting more stress events were more likely to develop a biologically verified cold, but infection was not inevitable, even for the stressed-out: About half of those with stress did not get sick.
2. The effect of stress events depends on where you are in life.
Just as some events are stressful, so are some nonevents — things that don’t happen when they’re supposed to in a typical course of life. People generally expect to graduate from school (high school or maybe college), get a job, get married, have kids and then retire. Failure to graduate, inability to get a job or rejection of marriage proposals can all be very stressful during the time of life when success at those things is expected. It may also be that different times of life are more susceptible than others to the ill effects of stress. Trauma in childhood, for instance, has been linked to higher risk of chronic diseases much later in life. Such trauma may induce long-lasting biological changes that contribute to disease in later years. In addition, “adversity during childhood may set an individual on a trajectory to being exposed to more stressors over the life course,” Cohen and coauthors write.
1. Stress doesn’t affect men and women equally.
Men and women respond differently to stress, both in their behavior and their physiological response. And women are apparently exposed more frequently to stressful experiences than men are. Partly that may be because “men tend to only report stressful events that occur directly to them” while women consider themselves stressed also when the actual event happens to someone close to them. Men and women may also differ in their vulnerability to stress-induced illness. Women seem more prone to stress-related depression, for instance.
Toll of stress on disease
All these “secrets” sketch a still incomplete picture of the stress-illness connection. Some things are clear: Evidence is strong that stressful events make a disease you already have worse, but the research is iffy about whether stress can make you sick to begin with. There are clues about how stressful events exacerbate disease — by altering your biology, your mood and your behavior. Chronic, ongoing stress (like working for a psychopath boss) generates a more general susceptibility to the kinds of physiological and emotional changes that promote disease, while acute immediate stressful events can be effective triggers for turning underlying conditions like cardiovascular disease into heart attacks.
Still many questions about the stress-disease relationship remain unanswered. Experts don’t even know exactly why stressful events are stressful. And evidence is meager on whether particular types of stress are especially likely to promote specific diseases. Much remains to be learned about how a stress event’s effects vary with your stage in life.
Nailing down those details remains a major research challenge. It’s not easy for researchers to answer all these questions, because the obvious experiments would be somewhat unethical. You’d have to give one big group of people a bad job with a bad boss and then make sure bad things happened to them all the time, while rigging conditions for another group to enjoy stress-free luxury. It would be kind of like The Truman Show, only with manipulating enough characters to get statistical significance.
Read More:
10.1146/knowable-083001-042301
https://www.annualreviews.org/doi/10.1146/annurev-psych-010418-102857
![]() This article first appeared in Knowable Magazine an independent journalistic endeavor from Annual Reviews and is republished here under a Creative Commons license.
This article first appeared in Knowable Magazine an independent journalistic endeavor from Annual Reviews and is republished here under a Creative Commons license.
Author:

Tom Siegfried
Tom Siegfried is a science writer and editor in the Washington, DC, area. He writes the Context blog for Science News and is at work on a book about the history of the multiverse.





